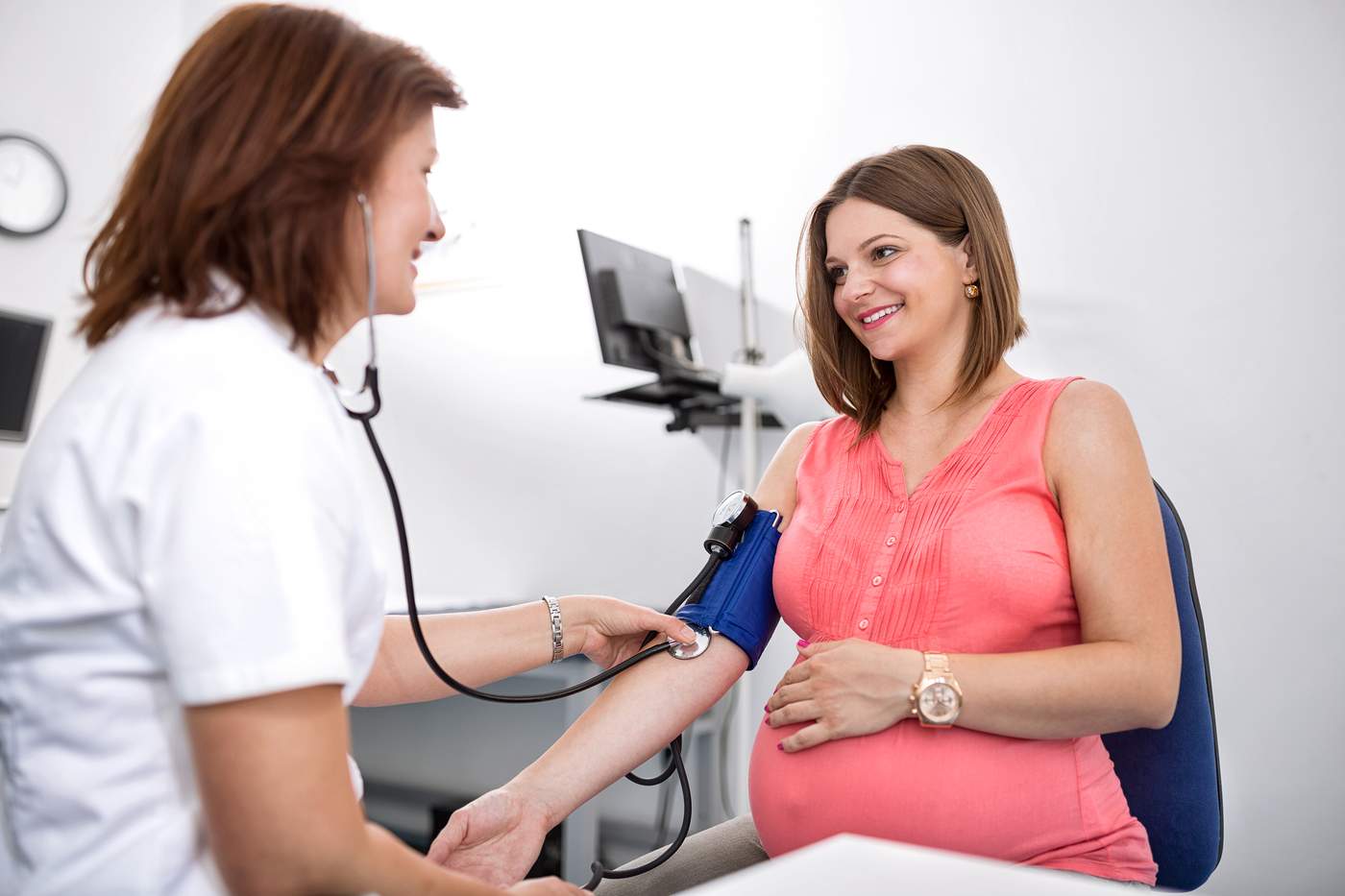
Women from the 1973-78 cohort of the Australian Longitudinal Study on Women's Health (also known as Women’s Health Australia) have responded to questions relating to pregnancy and postnatal health since Survey 2 in 2000. The information they’ve shared has contributed greatly to our knowledge of the emotional health challenges facing pregnant and postpartum women.
Using information provided by women in this cohort, researchers have been able to clearly identify risk factors for postnatal depression. These include mental health history, recent stressful life events and the lack of available social support (Chojenta et al., 2012).
The research also revealed that women’s emotional wellbeing during pregnancy is impacted by past pregnancy loss (either through miscarriage, still birth, ectopic pregnancy, or medical termination). Women who experienced a pregnancy loss were more likely to have depression, anxiety, low mood, and stress during subsequent pregnancies. However, the impact didn’t continue into the postpartum period (Chojenta et al., 2014).
References
AIHW: Humphrey MD, Bonello MR, Chughtai A, Macaldowie A, Harris K & Chambers GM 2015. Maternal deaths in Australia 2008–2012. Maternal deaths series no. 5. Cat. no. PER 70. Canberra: AIHW.
Austin M-P, Highet N, the Guideline Expert Advisory Committee. The beyondblue Clinical Practice Guidelines for Depression and Related Disorders — Anxiety, Bipolar Disorder and Puerperal Psychosis — in the Perinatal Period. A Guideline for Primary Care Health Professionals Providing Care in the Perinatal Period. Melbourne: beyondblue; 2011.
Austin M-P, Highet N, and the Expert Working Group. Effective Mental Health Care in the Perinatal Period: Australian Clinical Practice Guideline. Melbourne: COPE: Centre of Perinatal Excellence, 2017.
Chojenta C, Loxton D, Lucke J. How Do Previous Mental Health, Social Support, and Stressful Life Events Contribute to Postnatal Depression in a Representative Sample of Australian Women? Journal of Midwifery & Womens Health 2012; 57(2): 145-50.
Chojenta CL, Harris S, Reilly N, Forder P, Austin M-P, Loxton D. History of pregnancy loss increases the risk of mental health problems in subsequent pregnancies but not in the postpartum. PLoS One 2014; 9(4): e95038.
DoH. Changes to MBS items for obstetric services. Effective from 1 November 2017 (subject to passge of legislation). Canberra: Department of Health, Commonwealth of Australia, 2017.
PANDA. The cost of perinatal depression in Australia. Final Report Melbourne: Post and Antenatal Depression Association Inc (PANDA) & Deloitte Access Economics., 2012.
Reilly N, Harris S, Loxton D, Chojenta C, Forder P, Milgrom J, Austin M-P. Referral for management of emotional health issues during the perinatal period: does mental health assessment make a difference? Birth 2013 (a); 40(4): 297-306.
Reilly N, Harris S, Loxton D, Chojenta C, Forder P, Milgrom J, Austin M-P. Disparities in reported psychosocial assessment across public and private maternity settings: a national survey of women in Australia. BMC Public Health 2013 (b); 13:632
Reilly N, Harris S, Loxton D, Chojenta C, Forder P, Austin M-P. The impact of routine assessment of past or current mental health on help-seeking in the perinatal period. Women and Birth 2014; 27(4): e20-e7.
The research on which this report is based was conducted as part of the Australian Longitudinal Study on Women's Health by the University of Queensland and the University of Newcastle. We are grateful to the Australian Government Department of Health for funding and to the women who provided the survey data.